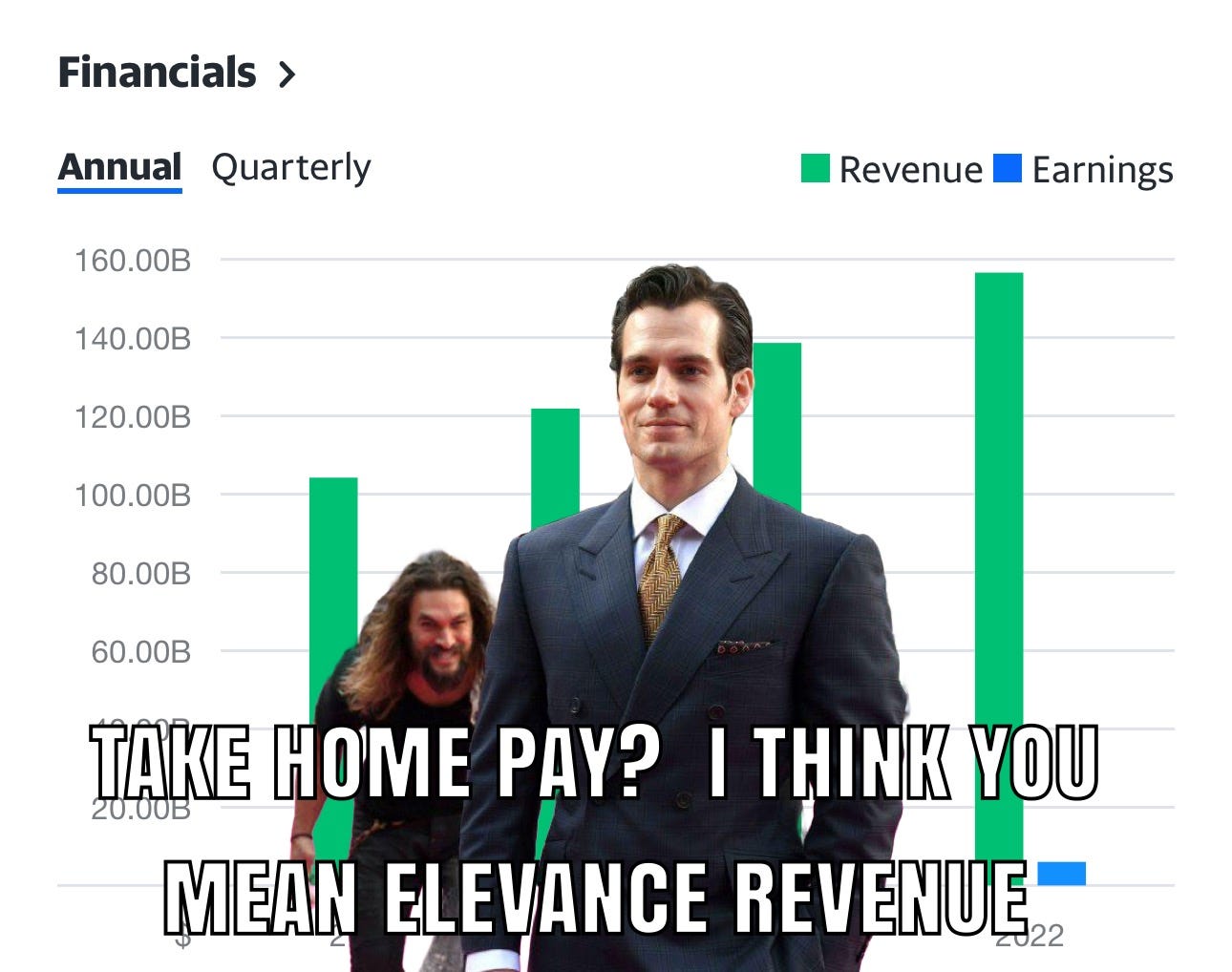
In Celebration of the Elevance / Anthem / Blue Cross Blue Shield / CarelonRx / Carelon Earnings Call!
Is it more important for big healthcare to intimidate customers than respond appropriately?
I am personally a dissatisfied customer. I am dissatisfied with a health insurance plan that happened to be my health insurance plan. This column details my relentless attempts to clarify why my health insurance plan decides to keep screwing with me as it relates to my medicine for psoriatic arthritis, in contrast to the fabulous shareholder value delivered by these efforts.
From yesterday's earnings call, Elevance Health1 was proud to announce the following:
“Our services business, Carelon, continues to produce results with double-digit top-line growth … as we continue to execute on our strategy of becoming a lifetime trusted health partner. Execution of our strategy is diversifying our revenue streams, creating greater earnings power and consistency in enabling us to deliver strong growth, regardless of the prevailing economic environment.”2
In recent years, employer-sponsored health insurance has become more of a burden for employers and patients. I have a plan provided by a company. I'm not sure what to call the company because it's got about 15 aliases. Is it a Blue?
I have psoriatic arthritis. I've written about this before. I take a medicine called Taltz. I would love to be taking another medicine. It is my doctor’s recommendation, called Xeljanz. But I can't afford it. I can only afford the Taltz because it's the only thing my insurance will theoretically cover. This leads to a lot of phone calls.
In fairness, I am a Compliance troll who lives under a bridge made of appropriate rules and regulations. I was trying to warn the company about the grave peril they face by not complying with all appropriate rules and regulations. In order to save everyone the trouble of having to read some recap of what a pharmacy benefit manager does, I have made this helpful-isn and concise video:
I have recorded six hours of telephonic communications with several entities, including, but not limited to CarelonRx, Carelon PBM, Elevance Health, and Anthem BCBS. I've done so well being told I was recorded and making it excruciatingly clear that I was also doing the recording on my side. Transcriptions of all of those phone calls will be made available. Here. It will embarrass all parties but only create liability for the plan.
For those unfamiliar, Elevance is a leading brand related to corporate fraud. That is not defamation; it is reporting: that's the federal government. It is actually just the federal government in one legal matter. There's also action by the Center for Medicare and Medicaid Services:



How much malfeasance are we talking about?
Well, at least since 2000, and this is only in publicly disclosed settlements, we're at about $600 million:
These violations range across a number of corporate activities…all of which are public!
I've dedicated at least six hours on the phone attempting—in the height of quixotic performance art—to secure responses from the pharmacy benefit manager, Carelon, and its specialty pharmacy, CarelonRx, both subsidiaries of a common parent entity. My principal query pertains to their justification for inflating the price of a medication beyond its actual cost whilst deceptively labeling it a 'discount'’
As I previously documented:
In contemplation of the complex operational structures of entities such as Anthem / Elevance / Carelon / Blue Cross Blue Shield, one may question whether they constitute legitimate businesses.3
This is not my question only…it’s that of the Ford Motor Company, for example.
After exhaustive endeavor hours of telephonic communications4, complemented by extensive electronic correspondence and social media engagement, all aimed at communicating with their corporate compliance department regarding a number of pertinent compliance issues5 and receiving no substantial response, one might reasonably speculate on the degree to which these entities take compliance nature.6
I propose the institution of a novel metric, akin to earnings-per-share, to scrutinize these corporations. Termed 'Earnings per fine' will enable tracking shareholder value vis-à-vis fraud.
It is noteworthy that, even with the total fines levied, since 2000, being deducted from this year's earnings-per-share, the figures still present a profitable7 picture.
However, my persistent efforts have ensured that the corporate compliance departments of these entities are perpetually aware of the issue above, thereby nullifying any potential for plausible deniability. This awareness is evident from my relentless communication with their corporate compliance departments, including but not limited to this selfsame article and additional communications.
As we progress, I anticipate their response to the classic query: "What did you know, and when did you know it?" will correlate with their interaction with my discourse on 'frontier psychiatrist substack,' which is not only amusing but discoverable, thus constituting a compliance issue.
Of significant concern, however, is the fact that CarelonRx has not made any provision for direct telephonic or electronic contact with their corporate compliance department, listing only a physical mailing address, as follows:
CarelonRx Compliance Coordinator
PO box 27401,
Mail Drop VA20023-N160
Richmond, Virginia 23279.8
But Before I Could Send My Complaint to Them…
Their external council reached out with this…
Ahem, And Now I Will Start Writing In Humorously Satirical Legalish Language to Underscore My Intent
In compliance with the request from CarelonRx, I will provide herein documented evidence of prior communication through their designated official channels. This contradicts the erroneous assertion by their legal counsel, stating that I left the communication to be incidentally discovered, which is false.
Furthermore, dear readers, anticipate the imminent publication of transcripts and audio records detailing extensive telephonic conversations in which I attempted to communicate my concerns directly to senior leadership to offer them the chance to protect themselves against the compliance issues presented. This attempt was both quixotic and calculated.
Enumerated Concerns:
My concerns center on the unpalatable and irrational delays experienced in my medical care, attributable to:
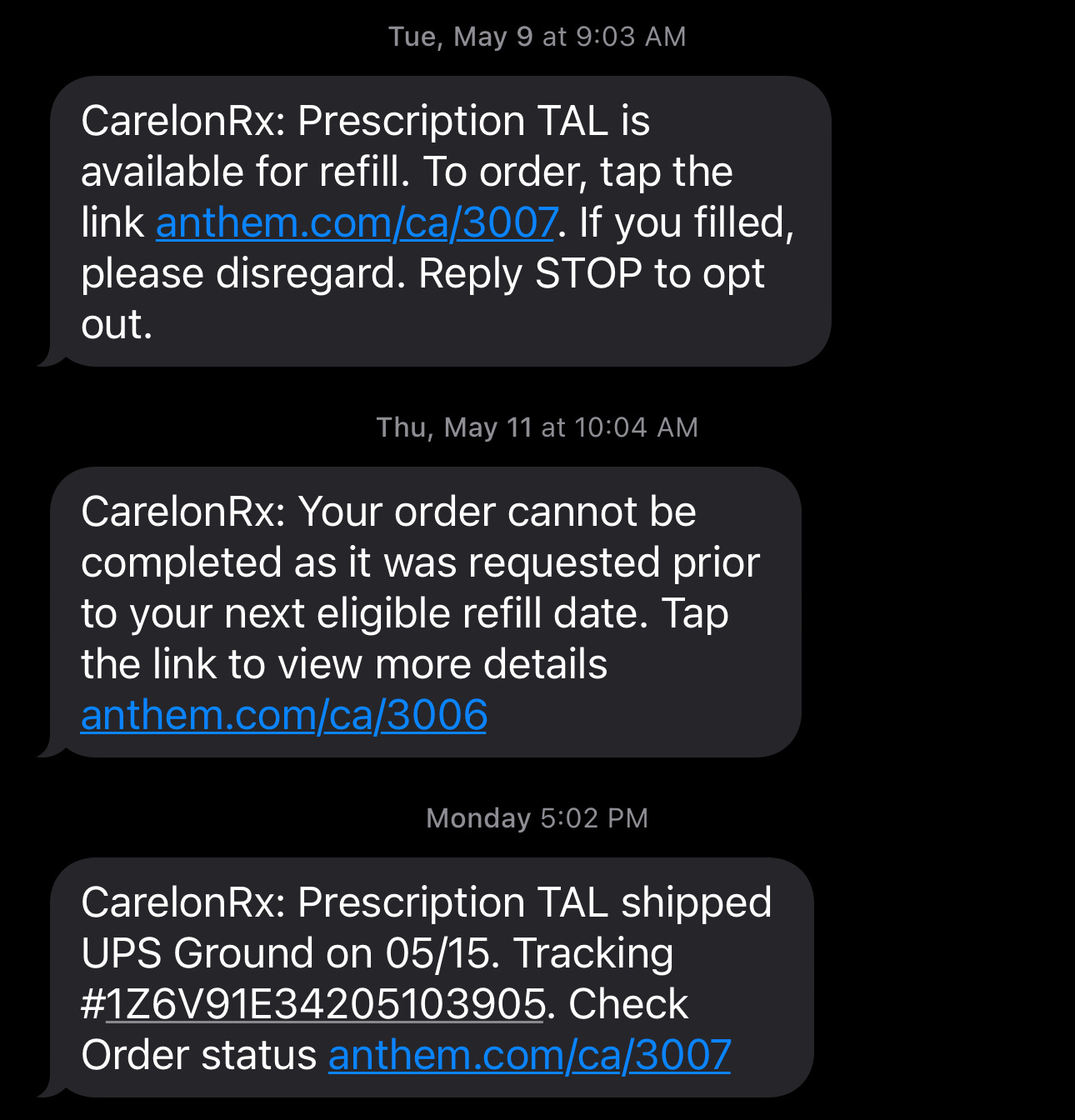
Misleading text messages regarding the status of my medication refills. These concerns were promptly reported to the plan sponsor and their benefits broker at the initial instance, to no avail.
I reference the sequence of text messages documenting the initial notification that my medication refill was ready, the subsequent message indicating it was not, and the egregious delay of seven full days between the initial notification and the actual delivery of my medication. Given the prescription regimen necessitates receiving this medication every 28 days, the resultant week-long delay has not only caused me undue hardship but also generated financial savings for your institution:
I affirm that my commentary on this matter was not solely confined to the Twitter platform. Indeed, I stand prepared to substantiate this. Furthermore, the referenced text message series is one instance among several such occurrences. This pattern has been recurring since my earnest attempts to report compliance issues to Carelon and CarelonRx, a process that has regrettably resulted in personal suffering.
Additionally, it must be noted that the aforementioned suffering is not abstract; it encompasses documented systemic inflammation. The resultant distress from your organization's actions has had such a deleterious impact that it has tangibly affected my Erythrocyte Sedimentation Rate (ESR), as observed in my recent medical results two days ago.
Despite my chronic autoimmune condition for which I'm receiving treatment with Taltz, I've never had an elevated ESR before this nonsense.
Let's continue…
Your letter today asserts that I did not contact CarelonRx other than by posting on Twitter. This is false and defamatory. I used multiple communication channels to report compliance issues at CarelonRx: Twitter, email, phone calls, and through articles in my newsletter, all of which were documented and provided to Carelon, etc. Despite the assertion in your letter from counsel, I've made 6 (six) phone calls to Carelon, repeatedly emphasizing my intent to report to protect senior leadership and Compliance. Moreover, I notified Carelon PBM Compliance, CarelonRx, Elevance, Anthem, the plan sponsor, the Benefits Broker, and the benefits consultant about these issues. Because Carelon's senior leadership subscribes to my newsletter, denial of awareness isn't viable. It raises questions about the inaccurate information your law firm was given regarding my actions. Ultimately, this evidence is discoverable, disproving your claim that I didn't use the appropriate channels.
Here's documentation of steps taken to contact Compliance at Carelon :
The first thing I did was send a complaint about the ADA compliance of your website. I received this response from Carelon confirming they had received my demand letter:
It is of significance to mention the date of March 16. It is worth noting I have an ocular issue thanks to my immune condition, which rendered this more than mere trolling.
I will include in this article the demand letter pertaining to the noncompliance of the Carelon website with the Accessibility Technology Act (ATA). Should any individual wish to pursue legal action against them for non-compliance with the Americans with Disabilities Act (ADA), they are fully within their legal rights to do so:
Following submitting the aforementioned demand letter, I received confirmation of its receipt. Their response was as dismissive as it was past appropriate statutory time frames:
Carelon Legal Responds to ADA Complaint 30 days Past Deadline to Dispute Claim...
My readers will recall that at the beginning of the automated compliance revolution I filed a complaint with Carelon for their ADA non compliant website… On March 16th (the same day of the demand letter for their ADA non compliant website) they responded:
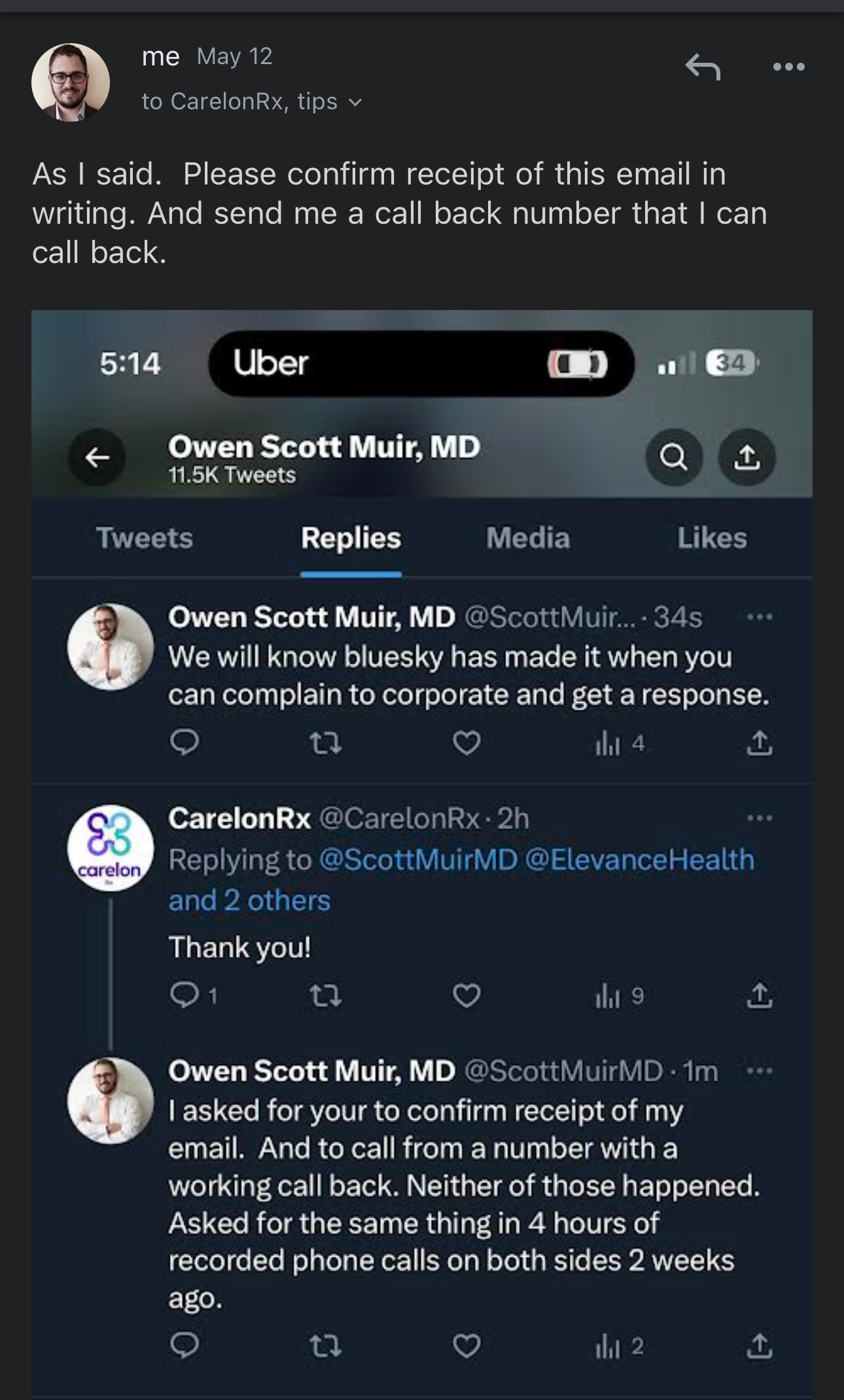
I took to Twitter to highlight the issue, initiated several telephonic conversations, and promptly emailed Carelon as their Twitter response unit advised.
It is unclear which leader of your organization engaged your legal services to engage me. I subsequently solicited written confirmation on May 12, which, as of the present moment, remains pending.
Contrarily, I received a letter:
This missive was from legal firm Troutman Pepper, asserting that I had not undertaken these aforementioned actions. This claim is not only inaccurate but also defamatory in nature. To wit:
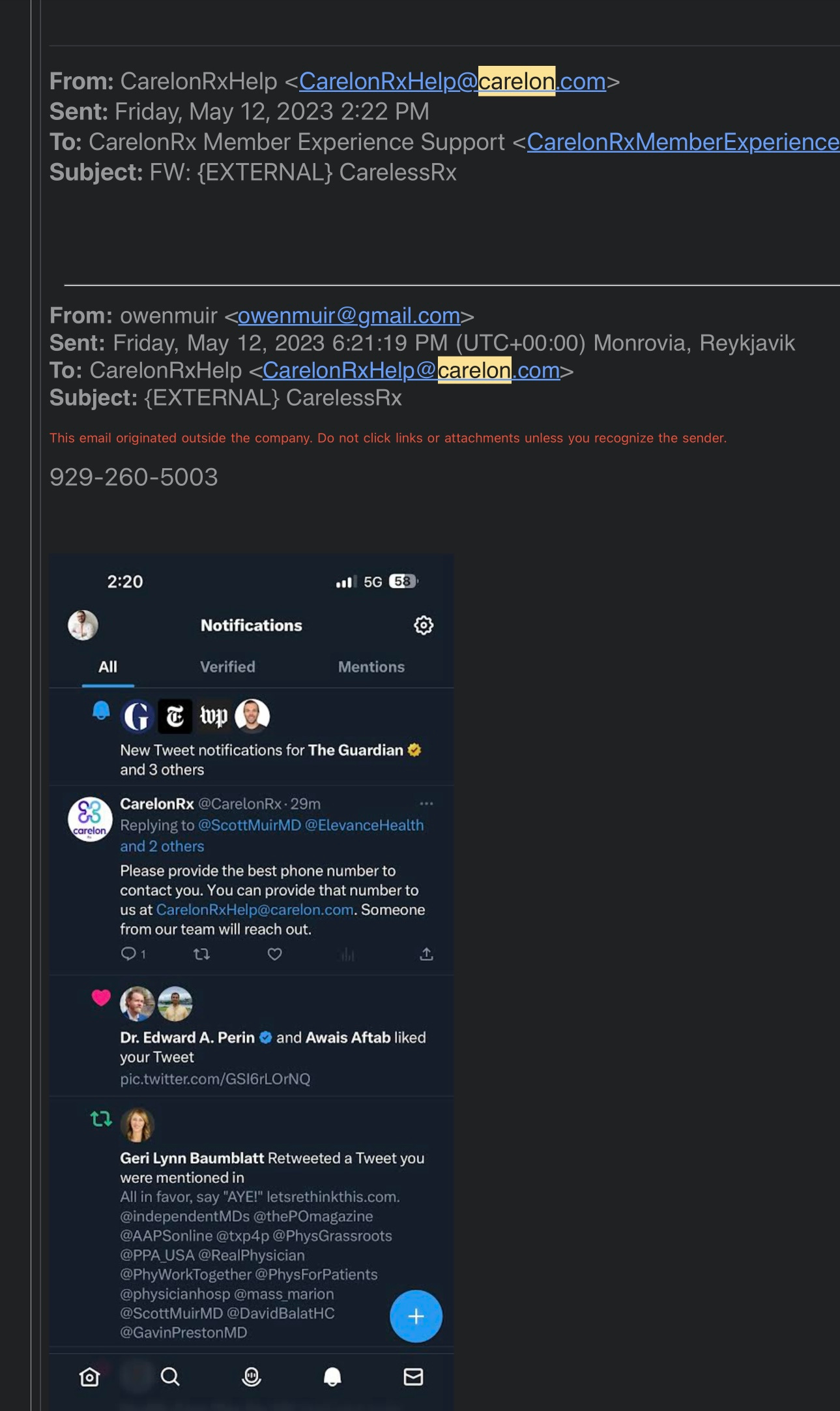
I will also provide the Twitter posts that led to the emails:
The aforementioned depicts by emailing a screenshot of the Twitter comments to Compliance and Carelon on May 12. This action starkly contrasts the narrative presented by Virginia Flynn, Esq. letter on behalf of Carelon.
Given Ms. Flynn is a partner in a consumer financial services department9, we are confronted with several unseemly possibilities.
Either Flynn's representation is knowingly false, another party misinformed her, or there was another failure. However, none of the presented options work was accurate10.
Flynn should know, per Troutman’s website:
She represents clients in federal and state court, trial and appellate level, in complex litigation and business disputes, health care litigation, including ERISA and out-of-network issues, and consumer litigation in more than 21 states nationwide.
Whichever the case, these circumstances are discoverable. Allow me to proceed:
Following the aforementioned events, I followed up with further communication on May 12 to provide all of the pertinent Twitter threads to the Compliance inbox, a fact that directly contradicts Flynn’s assertions— I honestly have a hard time from a satire and hubris standpoint comprehending this, BUT—her firm’s letter to me is addressed “Re: Your May 12, 2023 Complaint”.
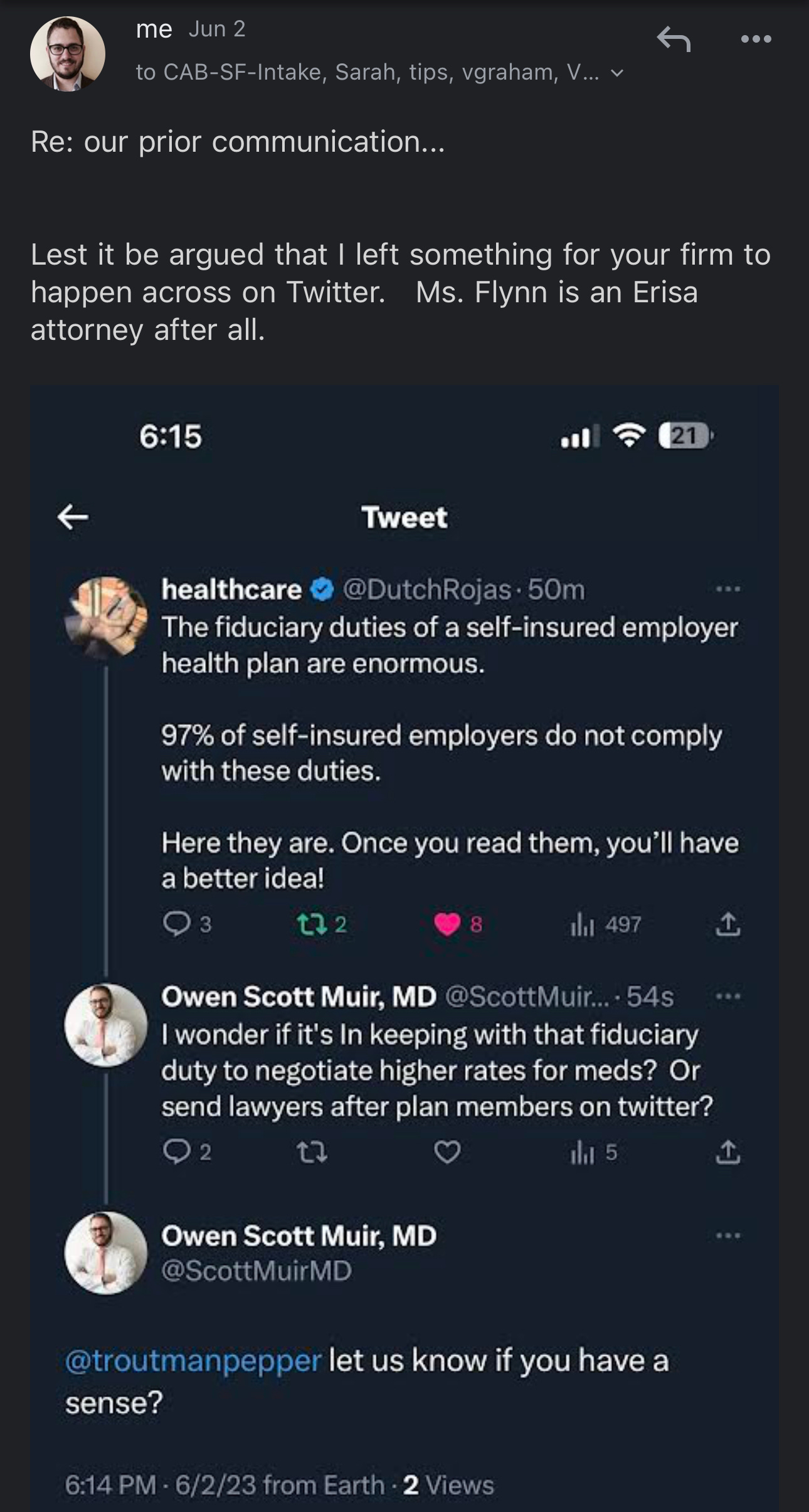
In that selfsame legal missive, dated May 18th, counsel asserted that I “hampered Carelon” by not “using official channels” and let them “happen upon” my complaints on Twitter. The four screenshots above alone are evidence to the contrary, but the phone calls…the phone calls….Ok.11
Attached is the article documenting that Taltz is one of two medications that work for me, and due to your punitive coverage policies, I cannot afford both. I have also composed an article outlining my medical journey with Psoriatic Arthritis, which I shall provide for your reference:
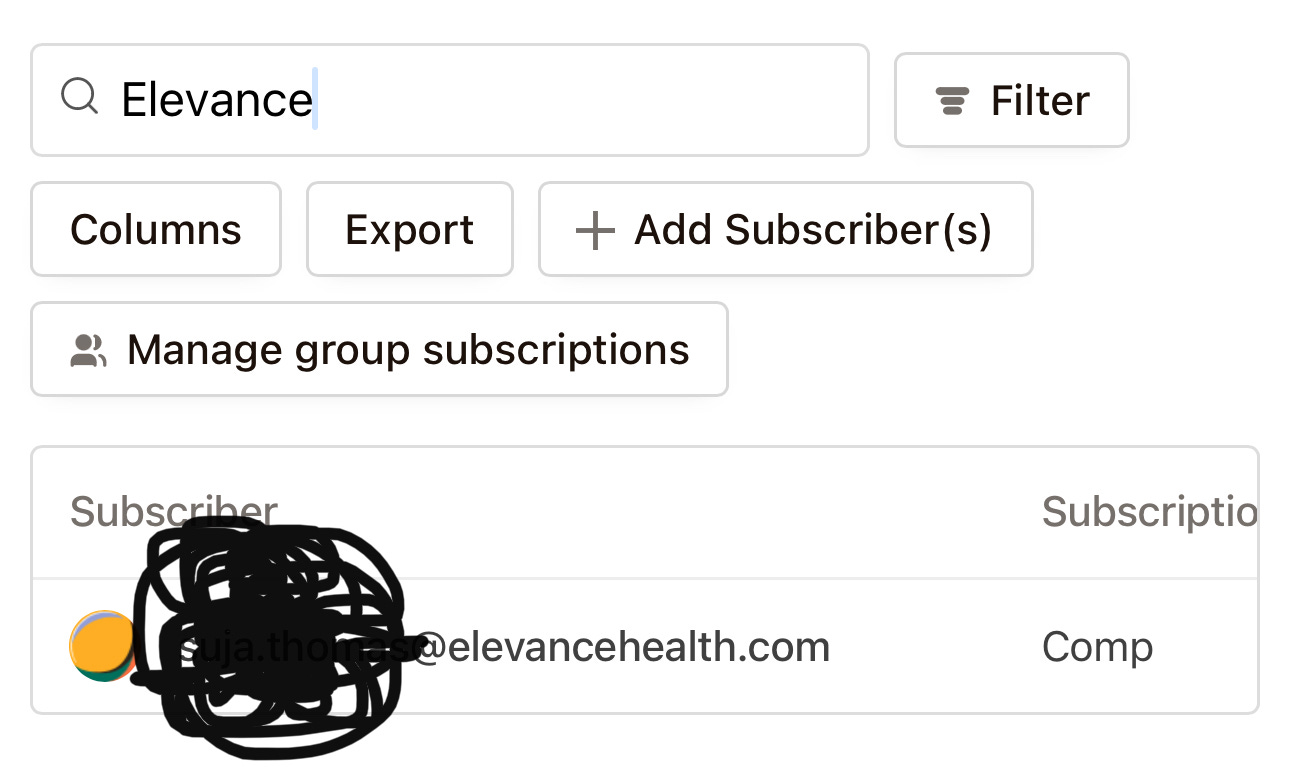
Although the documentation does refer to United Healthcare, it effectively outlines the entirety of the treatment assistance journey. It's also worth noting personnel from the Elevance team subscribe to this very newsletter:
Therefore, my compliance concerns are directly relayed to your inboxes with each issue's release. In due course, this fact will be corroborated during discovery when regulatory bodies begin investigating the complaints I have already initiated, as summarized hereunder:
This article in your inbox serves to document your notification about the following common issues with health coverage and encourages you to take action to preserve your compliance with all appropriate regulations.
Pharmacy benefits manager contracts that charge extravagant markups. If your members are paying more than they would with Mark Cuban’s CostPlus, CapitalRx, or any number of other options, you're out of compliance!
Here is that article for your convenience:
And the initial complaints were published— and emailed— to senior leadership at your company, who subscribe, with their corporate emails, to this very newsletter:
In making these statements, I am exercising my rights under the First Amendment of the United States Constitution to express my opinions and experiences. Any interpretation or representation in this correspondence is based on my understanding and personal experience. It is not intended to accuse any entity or individual of illegal conduct explicitly or implicitly unless stated otherwise.
Further, pursuant to the Communications Decency Act of 1996 provisions, particularly Section 230, I bear no legal liability for any third-party content referenced or included herein.
Additionally, any legal or factual assertions herein are made in good faith and are based on information available to me up to the present date, which is better than I can say for a partner at Troutman Pepper.
These assertions are subject to change in light of new evidence or further clarification of existing laws and regulations. I hereby reserve all rights and defenses available to me under the law.
This document does not constitute legal advice.
It is always advisable to consult with a professional legal advisor to understand your legal rights and responsibilities.
For purposes of consolidation and clarity
Please be apprised that the organizational structure whereby CarelonRx, a subsidiary of Carelon, itself a subsidiary of Elevance, all affiliated with Anthem BCBS, has been thoroughly examined and established. In accordance with my legal obligation, I have formally reported potential compliance infractions as a whistleblower. Both federally and in the state of California.
This declaration includes concerns relating to the failure of your company’s websites to meet the standards stipulated by the Americans with Disabilities Act, upon which I expounded in an article and received acknowledgment of receipt from your establishment. Furthermore, I endeavored to delineate the potential breach of fiduciary duty inherent in inflating costs on pharmaceuticals while erroneously terming it a 'discount.’ I imagine this concern would be relevant to Flynn, who defends clients from these allegations and commits coercive beeches of said rules at the behest of the same clients.
Additionally, I engaged in exhaustive dialogue with representatives of Carelon, Elevance, and CarelonRx, meticulously outlining my apprehensions as they intersected a plethora of regulatory issues. I utilized multiple communication channels, such as social media, journalism, email correspondence, and telephonic communication, to illuminate the aforementioned issues.
These actions were executed before my inaugural report to the Federal Trade Commission concerning their ongoing investigations into Pharmacy Benefit Managers (PBMs). They were also before my epic article on the topic of what I allege to be RICO-eligible PBM activity, as linked here:
SopranoRX: "Modern Gangsters"
“There used to be rules!” —Junior Soprano, fictional crime boss of the North Jersey Mafia on HBO’s “The Sopranos” Welcome to the Frontier Psychiatrists. What follows is one an ambitious pieces of writing. This took over three months and 50 hours to write. I’m a child and adult psychiatrist. I have come to believe understanding healthcare payments is the…
I emphatically refute allegations as factually false and defamatory and instrumental in perpetuating false statements made via the internet in furtherance of efforts to undermine customer free speech. I assert that utilizing digital communication to misrepresent business practices for financial gain is a serious matter.
Furthermore, I reject the notion that I evaded any calls. All telephonic interactions were duly recorded, amounting to six hours, the transcripts of which will be dispatched (and one included in the footnotes below), and the original audio is discoverable internally at Carelon.
It is also incumbent on me to express that could appear to be a coordinated campaign of retribution against a whistleblower. This would also be a serious matter. Given my disability status, this is a serious matter. I've addressed this legal issue previously:
A Case for Federal Racketeering Enforcement Against Utah for Anti-trans Hate Crimes?
The following is an argument. It’s an attempt to craft a legal rationale. I'm trying to provide some ammunition for legal scholars and advocates for trans kids. The right wing machine has done a phenomenal job of creating a worse world for vulnerable kids, and a worse world for the doctors who care for them. What follows is right out of the conserva…
In light of these circumstances, my course of action includes the publication of this article, followed by circulating it to all relevant parties and regulatory bodies, ensuring collective awareness. The transcription of all phone calls will follow. A sample is in the footnotes.
ADA complaints have, I will also note, been given a leg up recently with the 9-0 opinion in Perez v. Sturgis, as I wrote about in this missive, on June the 21st:
The ADA Compliant End of Life Quality Assurance Sphere Strikes Back!
“Regulators…we regulate any stealing of this property. And we are damn good too.” Rarely do I find myself pumping my fist in the air and silently mouthing “Yes, Justice Gorsuch, Yes!!!” Today is a rare exception. The Americans with Disabilities Act (ADA) of 1990 is crucial legislation for people with disabilities. As a child and adult psychiatrist, it is …
While I acknowledge sarcasm in my communications, I categorically reject the assertion of unprofessionalism as defamatory. I am a physician, and to my dismay, familiar with defamation law, and were any such allegation to be made publicly on the part of Troutman Pepper, as opposed to skewered in my own newsletter, it could be a serious matter. Again, I am free to make fun of myself all day long, but for others to take swings at me? Less clear, and the venue would matter.
As a patient, my professional obligations are toward patients. In this context, I am a physician, journalist, and patient. Therefore, the onus of professionalism lies on Troutman, Carelon, and its legal representation, a standard that appears not to have been met. I recommend thorough legal diligence be carried out before issuing threats to patients over the internet… not remotely in my fiduciary interest, and coercive12:
Upon a conviction for a willful violation of ERISA’s reporting and disclosure requirements, a fiduciary may be subject to fines and/or imprisonment for not more than ten years. There is also a provision in ERISA that applies to any person, not just ERISA fiduciaries, that makes coercive interference with ERISA rights a criminal offense punishable by fines and/or imprisonment for up to ten years. In addition, outside of ERISA, there are a number of criminal statutes that apply to any person, not just ERISA fiduciaries, including criminal statutes for embezzling from an ERISA plan, making false statements in ERISA documents, and taking illegal kickbacks in connection with an ERISA plan.
I did solicit a verbal callback from Flynn personally, left a Twitter comment, and proceeded to email it right back to Troutman Pepper just in case:
The absence of a returned call has been duly noted. Following the failure to receive a callback, I initiated reporting of this situation to the federal trade commission, who are currently investigating the role of PBMs:
From the June 6th press release from the FTC:
The largest PBMs are part of vertically integrated companies and act as middlemen and negotiate rebates and fees with drug manufacturers, create drug formularies (lists of medications that are covered by insurance) and policies, and reimburse pharmacies for patients’ prescriptions.
As part of its ongoing inquiry, the FTC issued similar compulsory orders on June 6, 2022 to the six largest PBMs: CVS Caremark; Express Scripts, Inc.; OptumRx, Inc.; Humana Pharmacy Solutions, Inc.; Prime Therapeutics LLC; and MedImpact Healthcare Systems, Inc.
The largest PBMs are integrated with the largest health insurance companies and wholly owned mail-order and specialty pharmacies. They influence which drugs are prescribed to patients, which pharmacies patients can use, and how much patients ultimately pay at the pharmacy counter. PBMs also have substantial influence over independent pharmacies, which have collectively voiced concern that PBMs negotiate and leverage contractual terms with these pharmacies that are confusing, unfair, arbitrary, and harmful to their businesses.
The FTC’s inquiry is aimed at shedding light on several PBM practices, including charging fees and clawbacks to unaffiliated pharmacies; steering patients towards PBM-owned pharmacies; potentially unfair auditing of unaffiliated pharmacies; the use of complicated and opaque pharmacy reimbursement methods; and negotiating rebates and fees with drug manufacturers that may skew the formulary incentives and impact the costs of prescription drugs to payers and patients.
This is of course on top of congressional inquiry:
The House Oversight and Accountability Committee is launching an investigation into pharmacy benefit managers over alleged anti-competitive tactics, according to a release from Chairman James Comer, R-Ky.
It’s the latest action targeting PBMs for allegedly using their market power to raise drug prices amid rising scrutiny, and comes as the Federal Trade Commission also launched a similar investigation.
Comer requested documentation regarding PBMs’ practices to determine how they are impacting healthcare programs administered by the federal government from the Office of Personnel Management, the CMS and the Defense Health Agency, according to a release.
Given the circumstances, I anticipate an apology and possibly more consequential rectification. I remind you that all interactions and correspondence are discoverable and thus contribute to the body of evidence described herein. This video with my daughter sums up the situation better than anything else I can do, and in much less time:
Sincerely,
—Owen Scott Muir, rheumatology patient, plan member, and satire-journalist. Also, a physician.
The stock price went up more than 4%.
From Cris Deacon at Versan Consulting…Translation = We want to be everything, to everyone, in every stage of life, so we have created companies to serve this purpose: home health, Rx services, specialty Rx services, mail order Rx, durable medical equipment, telemedicine, urgent care centers, payment integrity offerings, digital engagement tools - you name it we want to do it. We can make way more money if we are able to make $$$ outside of the MLR limits.
And when you control both sides of the equation – i.e., negotiating healthcare prices on behalf of our consumers and profiting from the prices we negotiate with ourselves – we can weather any economic storm or condition. After all, the bigger our piece of the pie gets, the more pie our shareholders get to eat!
or rather fall under the purview of illicit consortia?
One, just one of the calls, is transcribed, word for word, with very little editing for clarity. I’m in Italics, and the Carelon Reps are not. this is the second call on the above topic, but I recorded it, told them so, and ensured they understood the problem's nature…I included the time stamps out of a combination of grim humor and spite…[00:00:00] T A L T Z.
[robot] Sorry, if you are the patient, say yes or press How can I help you today?
Taltz prescription.
[robot] Which option would you like? Fill a prescription, check the status of an order, or do something else. To get you to the right person, say the medication you are calling about.
Taltz.
[robot] That was Taltz, right?
Yes.
[robot] Please hold while your call is transferred.
Hi, this is Robin with Carolina R. A. Specialty Pharmacy.
How can I help?
Hi there, this is Owen Muir. I'm a patient, I'm calling, and I'm super late on, my medication, and you just messaged me to call you, so I'm doing [00:01:00] that. I'm also recording this call, just so you know.
I'm sorry; what was your last name? My last name is Muir, M U I R.
And what was your first name?
O W E N.
What's your date of birth?
XXXXX
Right. Can you verify your zip
code? XXXX
Thank you for that.
And just for the Taltz?
Yep.
And I did what you asked and got the enrollment card for the savings program,
but there's no way to input it on the Sydney app. And I messaged it yesterday, and you didn't do anything about it. So I called this morning, and I didn't get a callback, and now I got a text, and so I'm calling you because I got the number in the text, and I'd like to get my Taltz filled, and I'd like to pay five dollars because I have the prescription savings card that I can now give you to fill that [00:02:00] prescription.
Do you have a BIN number?
Uh, I do. Uh, the BIN number is XXXXX
[00:03:00]
Alright, and what is the group
X
I think I'm missing a number. I'm going to repeat it back.
X
That's correct. Do you have an effective date?
Uh, 12, uh, no, I don't have an effective date. It should be now.
I have an expiration date.
Okay.
The expiration date is X
I'm just getting this saved, and I'm going to get everything processed, and we can pick up that copay. One moment. Yep.[00:04:00]
Insurance, now it's on Copay Assistance, and just about done. Yep.
Yep, after insurance, Copay, 250. And after we find Copay Assistance, you did bring it down to 5.
Yep. We are all set with that.
And I see an order scheduled. We just need to update that delivery date. Yep.
Alright, we have this delivered.
We can do Thursday, the 20th. Is that ok?
Yeah, sooner would be better, but yeah. I'm already two weeks
late on this prescription.
Yeah. [00:05:00]
I have additional questions that are uncomfortable for you, by the way—saving everything.
Saving.
Alright, so I'm just going, to sum up this order to make sure everything is good.
You'll be receiving these Taltz. Pre-filled auto-injector. One in a pack. 80 milligrams per milliliter. X.
And it is shipped to arrive on Thursday, April 20th, 2023. And no signature is required. Did [00:06:00] that all sound okay? Yep. I'll sit with it and see if you have some questions.
Yep, so I have two questions that are important. Uh, the first one is, can you provide me with a compelling rationale for why the following thing happened?
I got a text at 4. 03 p. m. on Thursday, March 16th, that said, we are ready to ship your medication. Sorry, is this the right thing
I, no, hold on, I have to go down. So, on April 10th, I got a, okay.
On April 6th, I got the following text message.
Prescription Taltz is available for refill at 9. 02 a. m. So I refilled it, and then at 4. 13
I got a message saying your order cannot be completed as it was requested prior to your next eligible refill date.
So why did I get a thing saying available for refill?[00:07:00]
And then when I ordered it, I was told it was not eligible for refill because it was before the date. If you're the one who sent me the text message that morning that said it was. Can you please answer that question? Yeah, I understand it. I know it's frustrating. No, it's not frustrating. It's a breach of fiduciary duty on the part of CarelonRX.
So I need an answer to that question. And if you need to bump me to management, please do so.
So, for that, it does; sometimes it does send it out a little too early. But yeah, I do see the text that you did receive for ready-for-refill. Yeah. Why do you send texts that things are ready for refill before they're ready for refill?
The only explanation I would possibly be able to give for that is it just wants you to go ahead kind of and get a schedule early just to make sure there'll be no delays.
And when I did that, it caused a delay of weeks because I was going to Costa Rica.[00:08:00]
And so I've been suffering for weeks now.
Yeah, I'm looking at the notes here.
Yeah.
Okay. Yeah, she was sick on the 6th. They did say it was refilled too soon, until April 9th. And with that... Because we couldn't process insurance again until the night, but it wouldn't pay through until then. And I'm seeing what happened after that. Let me see what happened.
We did get that co-pay, which was 250.
It looks like...
So I already paid for this.
So I already did this.
You should refund my money.
Thanks.
I'm sorry, I couldn't hear you. Could you say it again?
You need to refund my money. Because now I have that co pay card that you didn't tell me about before. And I paid it, but I don't have to. So you should give me $245 back.
Correct.
So for [00:09:00] the, to be refunded as far as the field for last month, for March.
Yeah.
But they were you; you were enrolled in the copay assistance program?
No, but you didn't tell me about it last month. You only told me about it this month. So I'd pay you then, and don't pay you now to see if we could, I might do a refund or like .
Yeah, no, I would, I, I'm gonna expect a refund because, There's additional, I mean, just take care of it. I don't want to go back and forth about it. I expect a refund and I expect an email about that refund. Because you should be aware that I filed a grievance and have received no response about that grievance about the non ADA compliance of your website.
And I put in a demand letter and have received no response to my legal complaint about the lack of accessibility to myself as a disabled person. trying to access your website, which is not compliant with the Americans with Disabilities Act, which is a little bit [00:10:00] surprising considering you're a healthcare company.
I know, I know, I know. This is Chelsea. The other thing I do need to ask you, from a legal standpoint, this is sad, I know Carelon says that the average retail price of Taltz is 13,836.44 and our discounted price is 6,777. 1. Is that correct? Is what Carelon tells me are you asserting as Carelon's representative that that is factual?
Pfft.
We're getting there. Sorry, Jeff.
About 13,000?
So, what Carelon says when you log into the Sydney app, which was acquired by Carelon, is that the following is the case. As asserted by CarelonRX, the average retail price is one thousand [00:11:00] three hun thirteen thousand, sorry. One thousand, oh, I wish.
Thirteen thousand eight hundred thirty-six dollars and forty-four cents is the claimed average retail price. Our discount price is six thousand seventy-seven dollars and forty-one cents. That is what it says. So, and is that, and then tells me I have a plan savings of $13,586 44 cents. Is that correct?
From Carelon perspective, to your understanding?
I wouldn't be able to give you the answer to that to that. I'm not sure.
No, this is on your website, and Carelon is my insurance. My insurance company owns you in this case. So my insurance and Carelon are the same holding company, which is CVS Caremark.
As far as the average cost of the medication, I wouldn't have [00:12:00] the answer to that, I'm not sure. Well, this is what it says on the website of Carelon.
So Carelon told me that the average retail price was 13,836.44, and the discounted price, which I mean “our,” meaning Carelon, is 6,777.41. And thus, I am saving 13,586.44 somehow because my insurance is paying 527. 41, and there is a copayment of 250.
Now, what I would like to ask is, that is interesting, but when you actually go to the website of Lilly, the manufacturer of the drug, The list price of Taltz is 6,586.40 per individual pen, which is of course, what I'm prescribed, and you're telling me that the discount price is [00:13:00] 6,777.41 which is more than the list price according to Eli Lilly. And then you advise me that given the average retail price is 13,000, which is, of course, much more than the actual list price of the drug.
I am saving a ton of money somehow, but actually, my insurance is paying more than the list price of the drug.
Mm-hmm.
And does that make any sense to you?
So for the, I understand what you're saying. Yeah. But as far as, like, do you give any explanation to that, or why we, I guess, maybe charge you, you know, a whole lot more than what the manufacturer cost is?
Yes. Yeah, is there a manager who can answer that question?
Mm-hmm.
There may be, I can get you over to someone who may,
Like our escalation team. Yes, please escalate me.
That would be awesome because it turns out this is a, yeah, this, this endangers the tax exempt status [00:14:00] of your company's benefits to the employer, so please escalate me.
Okay, yeah. Can I just put you on hold?
Yes, you can.
Thank you. I’m your customer service representative.
I'm the worst, is having the most, The worst day of her life using day. I don't even know if it's the worst. You might just be extremely confused right now; that’s what happens. But don't jack up the cost on me and pretend I'm not going to figure it out if you're harassing me to do your scam card, because that's what this is.
This is getting me to use the scam card so they get kickbacks moving around because they're legally able to do that. I have to assert I'm not on a government plan for this to be legal because if I were, it would be a crime. But since I'm not, they can do a thing that is otherwise a crime.
Isn't that hilarious?
[00:15:00] [00:16:00] [00:17:00].[00:18:00]
[00:19:00] Wait, I'm on a recording.
Thank you so much for holding. So I do have Bernard here.
Awesome. And thanks for calling CarelonRx Specialty Pharmacy.
No problem. Your day. Thanks. Hi. Hi. Hello, Mr. Muir. Hi,
Dr. Muir, Doctor. Dr. It's an honorific. Hi, I have a doctorate. I have a medical doctorate. Please use it. It's not Mr. You know that it's on the file.
Oh.
This is Bernard with Caroline Rx Specialty Pharmacy Resolutions team on a recorded line, Mr. Mur. Awesome. Yeah.
Dr. Muir, as I just said. Just now, doctor.
Oh, a medical doctor. Oh, Dr. Muir. I'm sorry. I didn't know if you were talking to me or not.
Yeah, no, I was talking to you.
Phone in and out there called me. I apologize.
Call me Mr. And I'm not a mister, I'm a doctor in this context. Okay, so here's the problem.
Caroline Rx has a problem, which is that, uh, my contention is that you're [00:20:00] lying to me. And by me, I mean me as a plan member of this plan, and I need an explanation from you about a pricing discrepancy and the data I was provided. Does that make sense?
It makes very much, Muir.
Awesome.
So, you, you, yeah.
Because, the pharmacy, I'm sorry. Yeah, Carelon, CarelonRx Specialty Pharmacy, formerly Ingenio R. X. was acquired by, uh, by Anthem, correct?
Yes.
Your company is a wholly owned subsidiary of Anthem.
Yeah, but us, the pharmacy, we don't have any control of the pricing.
Uh, I, I am aware that you don't have any control of the pricing. I'm asking you questions about the pricing as related to me from someone who works at the pharmacy, which is owned by Anthem, which is, which own, is owned by a pharmacy benefit manager.
Anthem is a subsidiary of, uh... Of [00:21:00] as the Blue Cross Blue Shield plan of what ?
Correct.
Right. Your associated pharmacy benefit manager is, so what I was gonna state is we do have a pharmacy benefit manager, which we would have to get, not the pharmacy.
Yeah, no, but you're, you're the pharmacy, but you're owned by your pharmacy benefit manager.
Dr. Muir, what I was trying to state is, I have to get our Pharmacy Benefits Manager on the line to discuss this.
Great, let's do it.
Us at Pharmacy don't have that information.
Yeah, can you do that?
On our end, I sure can.
Awesome. Excellent. Here, as well, can I place you on a brief hold?
Awesome, let's do it.
Thank you, Karen.[00:22:00]
[00:23:00] [00:24:00] [00:25:00]
Dr. Muir, I was holding, for that benefits manager. I just wanted to check in and let you know I'm still here with you, okay?
Got it, thanks. Thank you,
Callie.[00:26:00]
[00:27:00]
[00:28:00] [00:29:00] [00:30:00]
Yeah. But it took a second to get Imagine Alicia on my back line, but I was checking in with you while she pulled up your info.
Awesome.
If you don't mind, continue to hold for me.
I do mind because I have to be home for my children, and my wife is pestering me, but I've been on hold for so long that I don't want to stop it. So the sooner she can get on the line, the better.
Sure. Dr. Muir and, you know, I can always have someone give you a call back if …
Yeah. But that didn't happen this morning, so, no,
. Oh, if you don't mind [00:31:00] holding, I will give you an option.
I mean, I do, I do mind, and also, I'm going to because I don't have a choice.
Sure, Dr. Muir, I'm going to get Felicia here on the line, you know, pharmacy benefits management department, okay?
Yeah. Can we figure out just whatever it is and set it up correctly so it can work? Well, I would love to, but I think you're the one that did this. But, tell me how to unfuck it.
Try signing in with Owen.
Does Owen
mirror at Gmail? If you sign in with that, does it lead somewhere? Try that. Yeah, I don't want to do it right now. Okay. We don't have to do
it My brain hurts too. My brain hurts too. I'm very over it. My thinking
capacities are definitely... , so this is going to Frontier Psychiatrist Podcast Files.
Save. I do these videos on the website. It's very good. But if this looks good, I want to do more videos about TMS so we can send them to people. Mm hmm. Good idea. And then we have... I've [00:32:00] explained things in a way that is sendable, or on the websiteable, or et cetera, and I don't have to keep doing it. Right?
So this is a demo of me explaining something so we can explain things later. Blah blah blah.
I've actually developed sort of a pitch that I talk to clients
about with the TMS. It's much more simple than yours, which
is great. TMS reduces your symptoms in a much
[00:33:00]
[00:34:00] It's still, it's still Bernard, Dr. Muir. I'm still waiting for Alicia to get your information corrected. I just wanted to check in this time,
okay? Dr. Muir, I’m just getting it taken care of. That's it.
I appreciate your patience.[00:35:00]
[00:36:00]
[00:37:00] [00:38:00] [00:39:00]
Dr. Muir. Yes. Finally, for holding so patiently, I have Felicia on, no, excuse me, [00:40:00]
Felicia transferred me to Liv, last initial F, in our Pharmacy Benefits Management, Manager.
Awesome.
So, I finally got them on the line. I appreciate your patience while we did so.
Okay.
Great.
Now, uh, give me one second here, and I'mma gets, Liv F on the line.
Great
No. Mr. Muir, excuse me. Dr. Muir. Yes. This last disclosure and I know it's premature, and you may have heard it since you've been on the line a couple of times being transferred. Yep. Are you satisfied with the steps that I'm taking in involving your inquiry? Uh, yeah.
Yeah, I am.
Well, thank you for that, Dr. Muir. And like I said, I will get Liz on the line in our PBM department.
Thanks. Great.[00:41:00]
Hello? Hi there, my name is Elizabeth and I am your dedicated rep. Can you state your full name for me, please?
Sure, there. My name is Dr. Owen, O W E N Muir, M U I R. I am a plan member. My wife is an enrolled employee with this plan. And I have a question. About my, uh, my, my pricing of the Taltz.
Okay,
Alright. So I'm gonna start by giving you some. And what is a good callback number? No, you're going to, I'm, we're talking now. I'm sorry.
I'm, I was on hold for 30 minutes to talk to you. I'll give you the number but don't hang up on me. ]
Oh, wow. Yeah, wow. Uh, my number is [00:42:00] 929 260 5003.
I'm going to start by providing you with some information from your website, and I need you to confirm if the information from your website is the accurate information that your website is supposed to have.
Okay. Ready? So, the claimed cost breakdown regarding the medicine Taltz, is listed on, the Sydney app, which was acquired by CarelonRX, which was IngenioRX, which is a wholly-owned subsidiary. of Anthem, Blue Cross Blue Shield, in this, in California, tells me that the average retail price is $13,836.44 for one, one jab of, of Taltz.
And “our discount price,” and by our, I'm guessing that means CarelonRX, the pharmacy, which [00:43:00] is, having the Pricing information dictated by the pharmacy benefit manager. And what's the name of your pharmacy? Benefit manager?, CarelonRX. You are a wholly-owned subsidiary of Carelon. The PBM owns the pharmacy, CarelonRx.
Mm-hmm.
Or are you both, in turn, owned by Anthem?
Mm-hmm. We are CarlonRx.
Right. And so you, are CarelonRx; you’re owned. By Anthem, the insurance company.
Yes. We are part of Anthem. Yes. Right. So Anthem bought you and owned you.
So your share price is not independent. If Anthem has a, is a publicly-traded company, which it is, anything from CAR would be reported to Anthem. Sh, you know, shareholders, that's the value you're [00:44:00] generating is the shareholders of Anthem? Mm-hmm. , yeah. Okay. So it's an average retail price. 13, 836. 44 Our discount price, 6,077.41 Co insurance, zero. Co-payment, 250. Insurance pays, and by insurance, can you define what that insurance there is? That's 6, 527. 41 What you pay, 250. Plan savings is listed as somehow 13, 586. 44, and zero of that was applied to my deductible last month. , is that all in your understanding, correct?
Let's take a look, [00:45:00] Yeah. Yeah. You've got you, your plan is 250. Yep. All those numbers are correct. Okay. I see the numbers. Yep. Just like you see them. Yep.
And so I do have a question. I have an important question.
Mm-hmm.
Which is given the list price of the drug from Eli Lilly, 6,586. 40, I'm confused. As given that list price, why do you list our discount price as 6,777, which is more than the list price From the drug manufacturer?
Yeah, it says the Client has to pay 13,831.44. Cost allowed 6,777.41.
Right, and so That's the cost. [00:46:00] There's a cost submitted, meaning this is the ..Yes. This is the price.
Yeah, I know.
And then there's a cost allowed.
I know.
Which is the…
I know.
Which is the …Okay.
The role of a pharmacy benefit manager Is what, in your understanding.., do you do there? That price is concerning.
We don't set the prices. We don't.
So who sets the prices, in your understanding?
That is, that is between the manufacturer and Carelon.
Right. And so I told you what the manufacturer sets the prices list manufactured publicly as the price of their drug, which is to
mm-hmm.
To repeat from Eli Lilly's public website.The list price of Taltz is 6,586.40 you and I can both [00:47:00] agree is not the same number as the 6,777.41.
In fact, our discounted price of 6,777.41
is more dollars than the list price of 6, 586.40.
Yeah, the list price is going to be different from what the contracting price is. Yes, I, I, I, I, I, I am aware of that.
Between Carelon and the manufacturers.
Right,
and so my point is that the average retail price here is also a lie.
Right, 13,836. 44. is pulled from somewhere.
Where is that number pulled from?
It's cost submitted from the manufacturer.
So, why do you have an average but that’s?
That’s not correct.
[00:48:00] because the average retail price would be the average.
Mm-hmm.
And, you understand the average retail price is not what, just what the manufacturer says. It has to do with the national average drug acquisition cost plus whatever the markup is.
And, uh, so you're, you're taking, you know, what is essentially a, a, a, a list price, and you're marking it up for the average retail price, which is confusing because what you're presenting me is not the NADAC. It’s the, it's a, a, an average retail price, which it.
I can't find it anywhere.
Is there a retail price on that? Uh, what... On their website? Their website does not list a retail price because they're legal, their job is not to determine that. The retail price of any medicine is determined by the pharmacy and the pharmacy benefit manager hashing out whatever the kickback, sorry, [00:49:00] rebates are going to be. In your case, as a specialty pharmacy owned by its PBM, which is owned by its insurance company, the decisions around what that thing should cost are entirely within your purview.
Now, theoretically, the job of Anthem is to negotiate discounts on behalf of plan members to whom you have a fiduciary duty, or at least to whom the broker and plan sponsor has a fiduciary duty. To negotiate discounts for medicines and would you say that your discounted price of six thousand seven hundred seventy-seven dollars and forty-one cents. Down from what you're saying the average retail price of thirteen thousand eight hundred thirty-six dollars and forty-four cents is a good discount compared to the list price which is less than that. [00:50:00]
Hmm.
Did you do a good job negotiating a discount? If the discount is more than what you could go and buy the drug from the manufacturer for.
And that I would have to talk to my upper managers that is not...
I'm recording this call, by the way.
I only show what the prices are here.
I'm recording this call so you're aware. Because I'm a, I'm a physician, I'm also a citizen journalist, and the planned sponsor has a fiduciary duty under ERISA to me.
And what I'm asking is... How is it possible that your negotiated discount is more money, which is the opposite of the meaning of the word discount, than the actual list cost of the drug? How is that in my interest?
For the negotiated discount...
[00:51:00] Right, how is it in my interest... is higher?
Yes, that's correct.
Your negotiated discount price is higher than the list price of the drug. So the word discount, in this case, means the opposite. Right? It's more than the list price. It would be a negotiated increase.
Right.
And so, the negotiation you did made the cost more, not less. Do I understand that correctly?
So, Carelon, talk to CarelonRX. You have a good point. I do have a good point. It turns out it's an important point because the tax-exempt status of these benefits is dependent on fulfilling the plan sponsor and broker's fiduciary duty to me.
Do you know what a fiduciary duty is?
Yes, I do. Can you define it for me?
[00:52:00] Well, I believe this call; I believe I should probably escalate this call so that way you can have someone, a senior rep,
define the word fiduciary. Yeah, I'm sure we're going to get to that, but can you define the word fiduciary?
Fiduciary, I'm not a lawyer, I'm not, I, I, I do not understand what you're
Do you want me to define it so you can understand it?
Oh, you can go; go right ahead.
Okay. So fiduciaries have a role that involves trust, especially with regard to the relationship between a trustee and a beneficiary. In this case, the trustees, according to the Combined Appropriations Act of 2021. which took the language from ERISA, passed in 1974, as it related to employee benefits under 401k plans, and copy-pasted that [00:53:00] language to employee benefits as they relate to health benefits.
And so the fiduciary duty that the plan sponsor, aka my wife's CEO and CFO, have to me as a plan member, the beneficiary, Is that they have a duty to do things that are in my best interest. And so, as a manager of money for me, negotiating an increase in price is a dubious benefit in that it is not one.
And it turns out that the personal financial liability of this problem is visited, at least according to the Appropriations Act of 2021. The plan sponsor and the broker who sold them that plan, both have a personal liability for their fiduciary duty to me. And so by choosing a plan that they [00:54:00] have to attest at the end of 2023 on December 31st, they have to sign an attestation that what you're telling me isn't what you're doing.
Because the gag clause rule was also revoked. I wrote a whole article about this in my newsletter. Do you understand the problem?
Okay. Yeah, what is what is your expectation with this phone call? What is it that you would like to see?
What I would like to see is for you to say whatever you're going to say on your recorded line and me on my recorded line, podcast. That we had it, and no one can deny that we had it.
It's evidence.
Evidence.
Yes. That we are evidence of that, we're not That the plan [00:55:00] sponsor and broker Are charging more than a list price, and there is no plausible argument that this is in their fiduciary responsibility to me.
Ah, okay. It's a scam, what you're doing. Your company is a scam, owned by another scam, owned by another scam, and you routinely and systematically up-charge people, probably including yourself. And by the way, this also applies to you as an employee of this company. And they just always do this stuff.
I just caught an example of a gross... version of it, which is just super obvious because it's within the same drug. Usually, they do this by like denying one drug that's less expensive to mandate another more expensive drug. Carelon made the mistake of doing this pricing dance for someone who knows what they're looking at. and then you made me get a discount card, which is another way of moving around rebates, which is the other legal mandate that you're legally able to do that, which [00:56:00] would, in any other context, be an illegal kickback thanks to your safe harbor law. And the FTC is currently investigating, your company and a number of other companies for this very action.And so if you review some of the recent FTC advisories and, and statements on this topic, And recent Senate testimony, you'll see this is a hot topic. And so finding such an obvious fiduciary breach, a discount that's more than the list price, is just, it's, it's spicy.
And so, senior management, I would appreciate a call from you. Because what we're talking about is evidence that the tax-exempt status of the benefits that you're selling needs to be revoked.
Because this is tax fraud. Because the only way you get to be an employee tax-exempt benefit is by complying with 1974's ERISA, upon which MACRA, HIPAA, [00:57:00] HITECH, ACA, No Surprises, and finally the Combined Appropriations Act of 2021 were all based. And so the Fiduciary Duty Clause of ERISA, applies to all of those things, and that means that if you're not doing that, the tax-exempt status of the benefits not only creates personal liability for the broker who sold the plan and the person who bought it and they will be forced to take action and attest that they have taken action once they know this. And so the reason I'm recording it is so that they can know it. So that when they attest, they can't attest that this was in there, you know, they can't say that they didn't know this because they definitely will know this because I'm recording the fact that they're going to know this. And they read my newsletter, and I know that because they send me feedback about how great it is.
Okay.
You've done this with other patients of mine, I'm a doctor, you do this all the time, I mean, you're doing your job. I get that. You have a gig; you have to not get fired. That's what most people are doing in their jobs. , but it's important to [00:58:00]document when there are glitches in the matrix that are evidence of the underlying scam.
Does that make sense?
Yep.
Does that sound like it's worth 58 minutes of my time?
Probably.
Do you think it was worth 58 minutes of my time?
58 minutes? Yeah. Oh, wow.
Yeah, I have years of psoriatic
Is that how long were you?
I have psoriatic arthritis and I was denied this medication. I got an email, and I got a text message saying it was going to be, it was eligible for a refill. So I sent in the thing saying it should be refilled, and then I got another text message that evening; too late for me to get the drug before I went on a vacation to Costa Rica. So I've been crippled for the past several weeks because I don't have my medicine, and I don't have my other medicine because I legally, I can't afford it. I don't have the money. I'm a doctor, and I don't have the money for my medicine because you won't pay for both at once, and you won't send this on time [00:59:00] even when you tell me it's eligible.
Because what I was told is CarelonRX sends refill reminders about things being eligible for a refill before they're not eligible for a refill. Such that when I went to get it refilled, it wasn't refilled, which again, I would argue is not in my personal interest from a planned fiduciary.
You would understand why someone, question mark, might be upset about this, question mark.
Oh, absolutely. Yeah.
Did you know any of this, by the way?
I do. I do.
Did, did, was any of this?
I'm sorry?
Did you know any of this stuff? I wouldn't expect you to.
Uh, not entirely. Yeah, yeah. Not entirely.
So I write a newsletter about this, and you're free to read it because it's funny. it's called the Frontier Psychiatrist, and it's a substack and it is pretty funny. I do; I have a whole section now I'm doing about the Lord of the Rings essentially. - where I do compliance complaints about Sauron, uh, as a parody of what's [01:00:00] happening. Uh, while I was waiting for you in these 58 minutes, I was working on an incident report for my problematic one-to-one between the Lord of the Nazgûl and the Mouth of Sauron. That's, that's literally how I spend my time entertaining myself. Uh, which is lame, and I will admit to that freely. Readers of my newsletter include...
Frontier of a scientist?
The Frontier Psychiatrists.
I'm sorry?
The Frontier Psychiatrists.
Oh, psychiatrists.
Yeah, because I'm a psychiatrist.
Okay, okay.
One of the people who read my newsletter is a, is senior management in your organization. And I know that because they subscribe.
Yeah,
I know, right?
Uh,
so among my readers, I have senior management at Anthem, Elevance, CVS, and Cigna. I know they're Optum people, but they didn't use their corporate email, which is smart because I [01:01:00] bash them regularly. and I write about stuff. And, one of the things I write about is automating the resistance and using automated compliance solutions to blow this all up. and a bunch of other stuff like mental health care stuff. I even have a piece on National Gag Clause Remembrance Day,
uh,
This makes fun of the Group Health Plan Anti-Gag Clause Prohibition Compliance Attestation, which, as of December 31st, 2023, has to be attested to by all ERISA fiduciaries on nonfederal plans, grandfathered health plans, and ERISA plans, and they all have to attest on December 31st of the year that they haven't been asked to sign a thing by Anthem or anybody else that didn't allow Anthem to disclose to them the thing we're talking about. Because historically, they have had gag clauses and claimed this pricing information was proprietary, and that's [01:02:00] not fair.
And so now it's not fair, and it's not legal, and they have to attest that that didn't happen. And so, to ensure that attestation is ironclad, I'm making sure that they can't attest to something that isn't true, and then I went and wrote a whole parody song about, on them, based on Auld Lang Syne about this topic, because I'm that much of a nerd.
I know, right?
Yeah.
For Auld proprietary kickbacks, my dear, we’ll drink a cup of whiskey for Auld profitable agreements yet for the sake of what was a pretty sweet deal. And surely you will buy with the billions of dollars you put in your pockets over the course of the past 20 years. And surely I'll negotiate a complex arrangement with a safe harbor law to justify my acquisition.
We'll take an attestation of compliance yet for the sake of good old times. We, too, have padded each other's padded wallets. From 1974's ERISA till just before the Combined Appropriations Act passed in 2021. The regulations between us ebb and flow [01:03:00] since the days of old lang gag clauses. For old disclosures to be forgotten and never brought to mind, should old profits be forgotten for the stake of attestation requirements?
That's it. So, that's the point, if you were wondering. And I hope it was educational and mild to moderately entertaining and not too confrontational because that wasn't the point, but it is frustrating to me that I have to suffer so that Anthem can make money on a complicated kickback scheme that is legal but shouldn't be.
Okay. I will make a note of it here about your concerns.
Yep. And I would love to talk to senior management at Carelon about how they justify this on God’s green earth because... My planned sponsor is probably going to want to know, and legally, it has to be told.
True.
And if you want to email me the copy of the contracting [01:04:00] that specifies that all this is legit, I'm more than happy to review it before that call.
Oh, I don't have access to, ... Yeah, you would. Yeah, there are certain things that I have access to. Yeah, no, I know. There are certain things that Senior has access to. Yeah,
but I’m telling you that these are legally now public information. So, the fact that you don't have access to it is an example of the thing that I told you was a crime.
Isn't that fun?
That's not proprietary information anymore. Everyone has to be able to know that. That's what everyone has to attest to on December 31st of, 2023. That you did not hide that information either internally or from your clients. And my guess is you did because you don't know it internally.
Well, that we did.[01:05:00]
Yeah. Yeah, I know, right? I'm sure there is access somewhere.
Yeah, someone has access somewhere,
but the person who doesn't have access is me, and I'm the person to whom you have a fiduciary or at least to whom the plan sponsor has a fiduciary duty. Do you see the bind?
Okay. Yeah. Absolutely.
Okay, so when should I expect it? Does that mean I get with the senior manager?
When should I expect a call from the senior member? Uh, and how senior are we going to be talking? We're talking about senior management.
I would; I can transfer you over there.
Great.
And they will be able to help you.
I would encourage it if that's,
yeah, of course. If you, you know, if I were you, if I were you, you know, I, I would definitely, talk to them.
Yeah. Because I'm broke. So, yeah, go for it. Let's do it.
Okay, hang on. I'll be right back
Awesome.[01:06:00] [01:07:00] [01:08:00] [01:09:00]
Okay, Dr. Owen, Due to the fact that you are recording the call;
yeah, which is my legal right in the state
would not be able to speak to you.
so you're telling me that you can record the call.
I'm sorry.
I live in the state of New York, where that's legal. I didn't even have to disclose it, but I did. You're recording the call and telling me senior management is unwilling to talk to me because I am exercising my legal right, and so are you, to record this call.
That's what I've been informed.
So you've been informed by whom?
A senior member.
So you're telling me, You're telling me on a recorded phone call for both of us, which is, by the way, discoverable on your end, [01:10:00] and I have the public on my end. Yeah, you're telling me a senior management member, who you will not disclose the name or role of, informed you that they're unwilling to speak to me, a plan member, about increasing the cost of my medication over its list price.
And systematically denying me access to that medication for my condition, which you've also done because I'm recording it, which is a thing that you also assert a right to do at the same time. And I want to be crystal clear. They told you they won't speak to me because I do what you do whenever someone calls you.
Is that true?
That is correct.
What is the role of the senior... of the senior management member who gave you that information.
That is their protocol.
What is the role, not the name? I didn't ask you the name; what is the role [01:11:00] of the senior management member?
Senior member? Just a senior rep?
Senior rep.
Give me the role, of senior rep, in what entity?
Maybe you should call them back right now. Maybe you should call them back right now. And say what I said to them and reconsider if they'd like that policy to be the thing that everyone hears about. Because we just had that whole conversation. You understand how important this is. You understand the personal implications for my health.
And you understand the legal implications for your company. And what you're telling me is that they will neither speak to me nor tell me who they are? You ask them if that's what they want the world to hear. You ask them that. Please. I am done being nice.[01:12:00]
I'm getting with my supervisor.
Okay. I bet you are.
I am. I just sent her a message on my team. It is my protocol.
Yep.
To, reach up to upper management.
Do you know what the role of a physician is?
Absolutely. To dispense medication and take care of their patients.
The role of a physician is to know when to break protocol. This is one of those times.
We are trained to understand the root causes of problems. This is a root cause of dysfunction in our healthcare system.[01:13:00]
Alright. Getting a supervisor from the site here. Alright.
Let's see. Negotiating. Come on.[01:14:00]
Alright. Let's take
a look. Here we go. Higher than the list price. Okay. Okay. Alright. They're telling me
to. Call another senior. Alright, I'm going to call another senior. Another senior member.
Maybe she's... something. Alright, hang on just a second.[01:15:00] [01:16:00] [01:17:00]
Okay, Dr. Owen Muir, are you still with me?
I am.
Alright, well, I do thank you, and I appreciate your holding. I do apologize for the wait. I have a senior member on the line right now, and she will be able to
take over the call.
Great.
And, and assist you with your questions, okay?
Yep.
Thank you.
Thank you. Hi there, what's your name?
Hello?
[Carelon hangs up after 1 hour and 23 minutes]
Numerous authoritative bodies, including the Federal Trade Commission and the Center for Medicare and Medicaid Services, alongside numerous litigations under the Employee Retirement Income Security Act (ERISA), the Affordable Care Act (ACA), Medicare Access and CHIP Reauthorization Act (MACRA), the Health Information Technology for Economic and Clinical Health (HITECH) Act, California insurance law, and the combined appropriations act of 2021’s fiduciary rule, bring their practices into question.
These entities' habitual utilization of multiple brand names may confuse observers.
Until more rigorous enforcement of laws and the imposition of substantial financial penalties that will deter shareholders become a reality, such fraudulent practices may continue.
Thought I'd save my readers the trouble.
https://www.troutman.com/professionals/virginia-bell-flynn.html…and going after consumers on Twitter seems outside her wheelhouse?: Successfully represented Blue Cross Blue Shield of Georgia, Inc. (dba Anthem Blue Cross Blue Shield) in an ERISA § 1132(a) matter in the Central District of California. The plaintiff alleged Anthem improperly denied benefits relating to Proton Beam Radiation Therapy (PBRT) to treat his prostate cancer. The court confirmed that records evidenced Anthem’s reasonable review and proper reliance on its medical policies, guidelines, and literature, as required by the health benefits plan at issue, in denying the benefits at issue. The court further held that Anthem’s determination that the plan did not cover the plaintiff’s PBRT treatment was not an abuse of discretion. As such, the court entered judgment in Anthem’s favor. Loren Swearingen v. Westlake Health Care Plan, et al., 2:20-cv-02052-MCS-JEM (C.D. Cal. August 24, 2021).
Other than the sarcasm allegation. That is accurate, but as it applies to the social milieu of Twitter, it could be argued that this is both normative and protected by Federal Code Section 230. Further, given I write a newsletter featuring “satire” and “humor” as SEPARATE subsection tags, I think it’s also well within the domain as a satire and/or humor professional to use sarcasm in my professional role?
I’m going to compose myself and stop laughing.
It is of course not clear what the definition of coercive would be as it relates to these matters under the law, but given the state of New York, for example, has entire statutes designed to protect journalists from spurious lawsuits brought on under the context of defamation l—the “anti-SLAPP” provisions—it is not impossible to imagine that lawmakers could provide similar protections to NY State residents like myself were were to be engaged in journalism.